It is no surprise that long-term care (LTC) facilities are a breeding ground for COVID-19. However, Florida has taken preventative measures to protect vulnerable residents in these facilities. As of July 29, Florida’s LTC facilities have a COVID-19 testing positivity rate of 4.00% compared to the state’s overall 13.03%.
Florida’s LTC facilities house 140,296 elderly and disabled individuals. Many of these residents suffer from underlying medical conditions like Alzheimer’s disease and cancer, which drastically increases their risk of serious illness.
On March 15, Florida issued Dem Order No. 20-006 to prohibit visitation to all residential, skilled nursing, and LTC facilities for 30 days. The order was recently extended until Sep. 5.
Exposure is a concern for these facilities. There are a great deal of unknowns regarding the novel coronavirus pandemic. Asymptomatic spreaders or those with a mild case could unknowingly bring in the virus, spreading it like wildfire in areas with vulnerable residents.
“We’ve seen the tragic situation in Washington state at a nursing home there,” said Mary Mayhew, Florida’s secretary for the Agency for Health Care Administrations. “Florida will and must take every step to prevent real and potentially fatal threats to our elderly and senior populations and those with underlying health conditions.”
On May 5, Florida issued Emergency Rule 59AER20-1 to outline additional regulations regarding the return of COVID-19 positive residents to LTC facilities. The rule requires residents to test negative twice before reentering an LTC facility.
Two weeks ago, the rule was reversed.
Governor Ron DeSantis, R-Fl., ordered the establishment of COVID-19 isolation centers. These centers serve as quarantine zones for LTC residents who do not require hospital care but have not yet tested negative. There are currently 21 isolation centers throughout the state of Florida.
Florida’s death rate in nursing homes is 24.1 per 1,000 residents compared to Massachusetts’s 120.3 and New Jersey’s 116.2. DeSantis attributes Florida’s numbers to regulated transfers of COVID-19 positive residents.
Such transfers, of which more than 6,300 occurred in New York, are problematic; they can further the spread of the virus. In contrast to Florida, a New York state mandate by Governor Andrew Cuomo, D-NY, required LTC facilities to accept recovering COVID-19 residents even if they were still positive.
DeSantis said, “Florida’s approach was [to] avoid introducing the disease into long-term care facilities and we drew a very firm red line.” The Florida Health Care Association supported his response, citing the importance of preventing COVID-19 from entering LTC facilities.
One persistent issue is testing. The Agency for Health Care Administration (AHCA) issued an Emergency Rule that requires LTC staff to be tested twice per month. While this may help slow the spread, health professionals say it is not enough. Test results for staff are available within 24 to 48 hours, but staff continue to work during this window.
Evidence suggests infection rates could be lessened by giving staff raises in exchange for an agreement to work only one job. Caretakers with additional jobs are at a higher risk due to increased exposure. Once infected, they act as a vessel for the virus to travel through the community and into these facilities.
Currently, Florida provides the testing kits for biweekly testing of LTC staff. However, facilities worry Florida will stop providing testing kits in September.
Without these kits or additional federal funds, LTC facilities will struggle financially. Steve Bahmer, president and CEO of the industry group LeadingAge Florida, estimates costs between $25,000 and $300,000 per month for ongoing staff testing.
During a COVID-19 roundtable, Gov. DeSantis assured LTC facilities there are no plans to shift the cost of testing onto them. “We’re [testing] every staff member every two weeks, and that’s going to keep on going. We’ve not put any limitation on that,” DeSantis said.
Additionally, the Trump administration announced that the U.S. Department of Health and Human Services will devote $5 billion from the Coronavirus Aid, Relief, and Economic Security (CARES) Act to LTC facilities. These funds will aid the critical needs of LTC facilities by helping them hire additional staff and increase testing.
The fight against COVID-19 in LTC facilities has become a political issue. Critics claim Florida’s response has failed LTC residents, but the data suggests Florida has fared well comparatively. Florida is 28th in LTC deaths per capita. The top five states have three- to six-times more LTC deaths per capita than Florida.
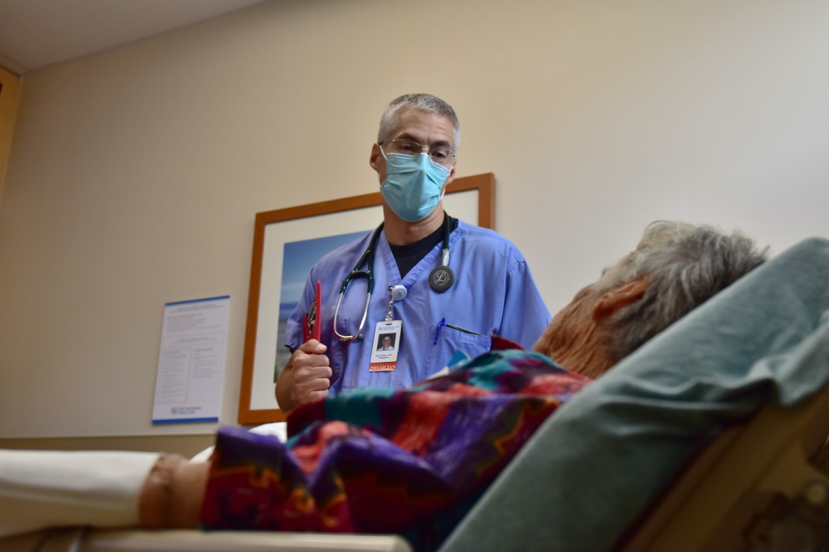
Featured image: An emergency room physician speaks with a patient in Panama City, FL on April 23, 2020. (U.S. Air Force photo by Senior Airman Dylan Gentile)